General Information
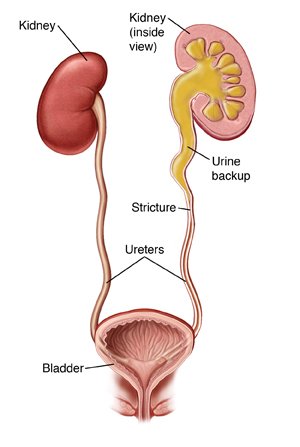
What is a ureteral stricture?
Ureteral stricture is a condition characterized by the narrowing of the ureter.
The ureter is the tube that carries urine from the kidney to the bladder.
This narrowing can restrict the normal flow of urine.
This can cause flank pain (pain in your back over your kidney), urinary tract infection, or kidney stones.
If left untreated, ureteral stricture may lead to loss of kidney function and shrinkage of the kidney.
Ureteral strictures may be caused by:
Previous surgeries or procedures involving the ureter.
Previous surgeries or procedures involving the other pelvic organs.
For example, treatment for cervical or rectal cancers.
Inflammation or scarring due to recurrent urinary tract infections.
Kidney stones that get stuck in the ureter.
Trauma or injury to the urinary tract.
How is a ureteral stricture diagnosed?
Kidney ultrasound to look for swelling of the kidney.
Renogram: this is a nuclear medicine study done to assess how well the kidneys are draining
It is also able to assess the differential function of each kidney (how much each kidney is contributing to the total workload) and where along the ureter the obstruction is, if present.
Ureteroscopy with retrograde pyelogram: this is a procedure that takes place in the operating room.
A tiny camera is inserted into the bladder and up into the ureter.
It is used to visualize the narrowing within the ureter.
Dye is inserted at this point and x-rays are taken to confirm the narrowing.
What are treatment options for ureteral stricture?
There are multiple methods for treating ureteral stricture, depending on the location and length of the narrowing. Often, we are not sure which method will be required until we begin the surgery.
The most common methods of repair are:
Primary ureteroplasty: in this technique, the area of narrowing is sharply incised longitudinally and closed transversely. This is best utilized for shorter strictures and when the tissue is mobile and healthy.
Oral mucosal graft ureteroplasty: this technique is best used when the stricture is greater than 2cm or when the healthy tissue is unable to be brought together to itself. Tissue is taken from the inside of the lower lip or the cheek and used to patch the ureter where it has been narrowed.
Ureteral reimplant: when the area of narrowing is at the point where the ureter enters the bladder, a simple reimplant may be the best option.
This involves transecting the ureter at the area of scar tissue, opening it up, and plugging it back in to the bladder at a different location.
This occasionally requires additional procedures to help mobilize the bladder such as a psoas hitch or Boari flap.
Pyeloplasty: this procedure describes reconstruction of the ureteropelvic junction, which is the point where the renal pelvis drains into the top of the ureter.
Similar techniques such as primary repair and use of oral mucosal graft may be utilized in this location as well.
Other options include ileal ureter and ureterocalycostomy. These are less often necessary and your surgeon will specifically mention these if you may be a candidate.
Ureteral repair at our institution is done using the surgical robot. You will have 1-2 small incisions in your abdomen.
After the repair is complete, a small plastic stent is placed within the ureter to facilitate healing.
primary repair
oral mucosal graft
Post-Operative Instructions
***DISCLAIMER***
The below instructions are provided to Dr Alford’s patients. If you are undergoing a procedure with a different surgeon, please follow the discharge instructions that were given to you at discharge.
Wound Care
Your incisions are closed with skin glue and sutures.
The sutures will dissolve with time and do not need to be removed.
The glue will come off on its own and does not need removal.
You may shower the day after surgery.
Let warm soapy water run over your incisions.
Do not scrub your incisions, and be sure to pat your skin gently to dry after the shower.
Do not take baths or swim for 2 weeks after surgery.
Medications
Take all prescriptions as prescribed.
Take over-the-counter tylenol and ibuprofen as first-line treatment for pain.
You will be prescribed a limited number of narcotics, these are for breakthrough pain.
Do not drive, operate heavy machinery, or drink alcohol while taking narcotic pain medications.
Take a daily stool softener for at least 1 week after surgery.
Constipation is very common after surgery and when you are taking narcotic pain medicine.
Try not to strain.
Diet
Your appetite may be low after surgery and recover over the first 1-2 weeks.
You can eat regular food without restriction, though starting with light and bland foods can be gentler on your stomach.
If taking narcotic pain medications, do not drink alcohol or take other sedating medications (such as benzodiazepines) as this can slow your breathing.
Activity
Do not lift anything heavier than 10 pounds and no strenuous or vigorous activity for 2 weeks after surgery.
Avoid activities that increase the pressure inside your abdomen, such as straining for a bowel movement or ab exercises.
It is very important to remain active after surgery - avoid sitting for long periods of time.
It is dangerous to sit for too long after surgery - you can develop blood clots in your legs and lung infections.
Take short, gentle walks frequently during the day while you recover.
Stairs are fine.
Catheter Care
Not every patient requires placement of a catheter after this type of surgery.
Catheters can cause urge sensations as well as bladder spasms; this can be caused by the balloon that keeps it in place and is normal. Sometimes this sensation can cause leakage of urine around the catheter. As long as most of your urine drains through the catheter bag, this is not concerning.
If your catheter stops draining, you are having bloody urine with clots, or are having significant discomfort, please call the office or go to the emergency room for evaluation.
If you go to the ER for evaluation, let them know you had a urology surgery and that they need to discuss any changes to your catheter with your urology team as the catheter may be in place to help parts of your body that were connected by the surgery heal appropriately.
Stent Care
The stent inside your ureter is completely inside your body, you will not see any part of it.
It is very common to experience urinary urgency and frequency, blood in the urine, and pain in the kidneys while voiding when you have a stent in place.
These symptoms will resolve when the stent is removed.
Follow-Up Appointments
You will have a stent placed inside your ureter to help the repair heal.
It will be removed in the office 2 weeks after surgery.
If you have a nephrostomy tube, it will be capped. Keep it capped throughout your recovery unless you experience severe flank pain, fevers, or chills.
The nephrostomy tube will come out 1 week after stent removal.
If you have a catheter draining your urine, will come out 2 weeks after surgery.
Follow up with an ultrasound of your kidneys 1 month after tube removal and then every 6-12 months for at least 2 years.
Literature Review
Robotic ureteral reconstruction for recurrent strictures after prior failed management. Lee et al, 2023.
CORRUS study.
105 patients with recurrent ureteral stricture who had failed prior endoscopic and/or surgical repair.
Median stricture length of 2 cm.
Variety of robotic techniques may be utilized, depending on etiology and location of stricture.
Buccal mucosal ureteroplasty for the management of ureteral strictures: patient selection and considerations. Gonzalez et al, 2022.
When to consider primary use of BMG.
Contraindications.
Robotic ureteroplasty with appendiceal onlay flap: an update on the outcomes of 18-month follow-up. Wang et al, 2022.
8 patients with average stricture length of 4.3cm.
All right sided (must be right sided to use appendix).
At follow-up of 18 months, no patients had needed any additional procedures.
Robotic ureteral reconstruction in patients with radiation-induced ureteral strictures. Asghar et al, 2021.
CORRUS study.
32 patients with 35 ureteral strictures (median stricture length 2.5 cm).
Techniques performed included reimplantation (29), appendiceal onlay (4), buccal mucosa graft (1), ileal ureter (1).
At a median follow-up of 13 months, 88.2% clinical and symptomatic success rate.
Robotic ureteral reconstruction. Drain et al, 2021.
Review of techniques that may be used to treat ureteral stricture.
Reimplantation, psoas hitch, boari flap, ureteroureterostomy, appendiceal flap, oral mucosal graft onlay, ileal ureter, autotransplantation.
Validation of robotic-assisted ureteroplasty with buccal mucosal graft for stricture at the proximal and middle ureters: the first comparative study. Yang et al, 2021.
29 patients with median length stricture of 3.1cm.
97% of patients experienced resolution of their hydronephrosis within 6 weeks of surgery.
A multi-institutional experience with robotic ureteroplasty with buccal mucosal graft: an updated analysis of intermediate-term outcomes. Lee et al, 2021.
CORRUS study.
54 patients with median stricture length of 3cm.
At median follow-up of 27.5 months, 87% were clinically and radiologically successful.
Ureteral rest is associated with improved outcomes in patients undergoing robotic ureteral reconstruction of proximal and middle ureteral strictures. Lee et al, 2021.
Ureteral rest is defined as absence of hardware spanning the length of a stricture for at least 4 weeks prior to surgery.
Includes ureteral stent and nephroureteral stent.
Higher rates of success and lower blood loss for those without a stent.
Multi-institutional experience comparing outcomes of adult patients undergoing secondary vs primary robotic pyeloplasty. Lee et al, 2020.
CORRUS study.
Revision pyeloplasty is associated with higher blood loss and longer operative time.
No difference in major complications or in overall success rate.
Revision surgery is more likely to utilize buccal mucosa graft.
A multi-institutional experience with robotic appendiceal ureteroplasty. Jun et al, 2020.
CORRUS study.
13 patients with average stricture length of 6.5cm (all right sided).
8 underwent appendiceal onlay.
5 underwent appendiceal interposition.
At mean follow-up of 14.6 months, 92% of patients had not required any additional procedures.
Robotic ureteral reconstruction using buccal mucosal grafts: a multi-institutional experience. Zhao et al, 2018.
CORRUS study.
19 patients with median stricture length of 4 cm.
53% of these patients had prior failed surgery.
At median follow-up of 26 months, 90% overall success rate.
Robotic ureteroplasty with buccal mucosa graft for the management of complex ureteral strictures. Lee et al, 2017.
12 patients with median stricture length of 3cm.
2/3 of these had previously undergone failed reconstruction.
At median follow-up of 13 months, 83.3% were clinically and radiologically successful.
Outcomes of robotic-assisted laparoscopic upper urinary tract reconstruction: 250 consecutive patients. Marien et al, 2015. `
250 patients undergoing robotic reconstructive surgery.
Techniques included pyeloplasty, ureterolysis, ureteroureterostomy, ureterocalicostomy, ureteropyelostomy, reimplantation, and buccal mucosal graft ureteroplasty.
Overall 98% radiographic success rate and 97% symptomatic success rate.
Range from 85% to 100% for individual procedures.
Robotic-assisted ureteral reconstruction using buccal mucosa. Zhao et al, 2015.
First published series of this technique.
4 patients with stricture length ranging from 1.5cm to 6cm.
At follow-up of 10.7 to 18.6 months, 100% radiographic success.